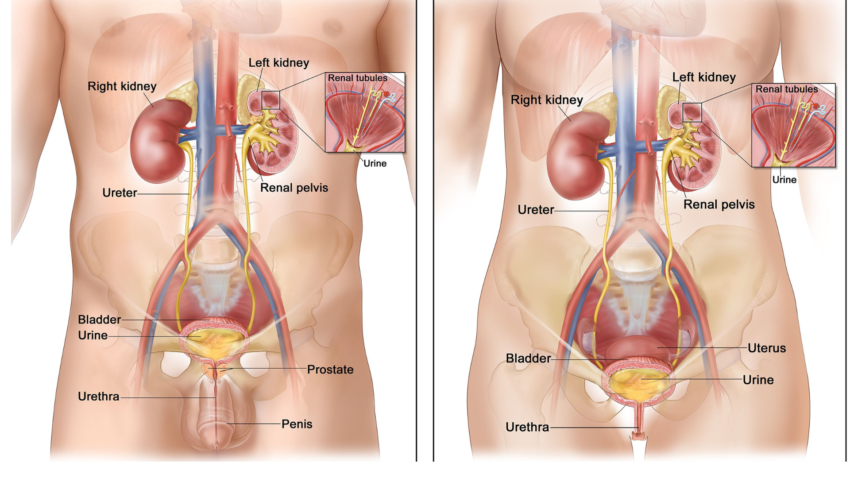
Metastatic Bladder Cancer
Bladder cancer is a significant health concern, and when it advances to metastatic bladder cancer, the disease becomes even more challenging to treat. Metastatic bladder cancer occurs when cancer cells from the bladder spread to other parts of the body, such as the bones, liver, or lungs. This progression complicates treatment and significantly impacts the patient’s prognosis and quality of life.
What is Metastatic Bladder Cancer?
Metastatic bladder cancer is an advanced stage of bladder cancer where the cancerous cells have spread beyond the bladder to distant organs. This type of cancer typically starts in the cells lining the bladder, known as urothelial cells. As the cancer grows, it can invade more profound layers of the bladder wall and eventually reach the lymphatic system or bloodstream, facilitating its spread to other parts of the body.
How Common is Metastatic Bladder Cancer?
Bladder cancer is the tenth most common cancer worldwide, with an estimated 573,000 new cases and 213,000 deaths in 2020 alone. The likelihood of bladder cancer becoming metastatic depends on various factors, including the stage at diagnosis, tumor grade, and the patient’s overall health.

Importance of Early Detection
Early detection of bladder cancer is crucial for improving treatment outcomes and survival rates. When diagnosed at an early stage, bladder cancer is typically confined to the bladder lining and has not yet invaded deeper tissues or spread to other parts of the body. Treatment options are more effective at this stage, and the likelihood of remission is higher.
Several factors contribute to the early detection of bladder cancer. One of the most common early symptoms is hematuria, or blood in the urine, which should prompt immediate medical evaluation. Other symptoms, such as frequent urination, pain during urination, and lower back pain, should also be investigated promptly.
Causes and Risk Factors
Metastatic bladder cancer can result from a combination of genetic, environmental, and lifestyle factors. Smoking is the most significant risk factor, increasing the likelihood of bladder cancer due to carcinogens in tobacco. Exposure to industrial chemicals, such as those used in the rubber, dye, and leather industries, also raises the risk.
Genetic Predisposition
Genetic factors can play a significant role in bladder cancer development. Specific inherited genetic mutations can increase an individual’s risk of developing the disease. For instance, mutations in the TP53 and RB1 genes involved in cell cycle regulation and tumor suppression have been linked to an increased risk of bladder cancer. Understanding one’s genetic predisposition can help assess the risk and take preventive measures.
Environmental and Lifestyle Factors
Environmental and lifestyle factors also contribute to the development of bladder cancer. Exposure to carcinogens, such as those found in tobacco smoke, industrial chemicals, and certain dyes, is a well-known risk factor. Smoking is the most significant lifestyle-related risk factor, with smokers being several times more likely to develop bladder cancer than non-smokers. Occupational exposure to chemicals in industries such as rubber, leather, and textiles can also increase the risk.
Associated Health Conditions
Certain health conditions are associated with an increased risk of bladder cancer. Chronic bladder inflammation, often caused by urinary infections or long-term catheter use, can contribute to the development of cancer. Moreover, individuals with a history of bladder cancer are at a higher risk of recurrence and metastasis. It is essential to monitor and manage these conditions to reduce the risk of developing metastatic bladder cancer.
Symptoms and Warning Signs
- Blood in the Urine (Hematuria): One of the most common early signs of bladder cancer is blood in the urine, which may appear pink, red, or cola-colored.
- Frequent or Painful Urination: Patients may experience an increased need to urinate, pain or burning during urination, and a feeling of incomplete bladder emptying.
- Lower Back Pain: As the cancer progresses, it may cause persistent pain in the lower back or pelvis, primarily if it has spread to nearby tissues or organs.
Common Symptoms
The symptoms of bladder cancer can vary depending on the stage and extent of the disease. In its early stages, bladder cancer may cause symptoms such as blood in the urine (hematuria), which can be visible or microscopic. Other common symptoms include frequent urination, pain or burning during urination, and a feeling of incomplete bladder emptying.
Advanced Symptoms
As bladder cancer progresses and metastasizes, additional symptoms may arise. These include lower back pain, weight loss, fatigue, and leg swelling. When the cancer spreads to other organs, it can cause symptoms specific to those areas, such as bone pain if it spreads to the bones or jaundice if it spreads to the liver.
When to Seek Medical Advice
It is crucial to seek medical advice if you experience any persistent or unusual symptoms that could indicate bladder cancer. Early determination and treatment are essential for further developing results. If you notice blood in your urine, experience pain during urination, or have any other concerning symptoms, consult a healthcare professional promptly.
Diagnostic Procedures
Initial Assessment
The diagnostic process for metastatic bladder cancer typically begins with a thorough medical history and physical examination. The healthcare provider will inquire about symptoms, risk factors, and family history during the initial assessment. This information helps in guiding further diagnostic tests.
Imaging Techniques
Imaging techniques play a crucial role in diagnosing and staging metastatic bladder cancer. Standard methods include computed tomography (CT) scans, magnetic resonance imaging (MRI), and positron emission tomography (PET) scans. These imaging modalities help visualize the primary tumor and detect any metastasis to other organs.
Biopsy and Histological Examination
A biopsy involves obtaining a tissue sample from the bladder or metastatic site for histological examination. This procedure helps confirm the diagnosis and determine the cancer’s type and grade. The biopsy results provide essential information for developing an appropriate treatment plan. Also, visit my other post. Mastering Ultrasound Tech.
Staging and Grading of Metastatic Bladder Cancer
Understanding Stages
Staging bladder cancer is based on the extent of the tumor’s spread. The TNM (Tumor, Node, Metastasis) staging system is commonly used to describe the cancer’s stage. T refers to the size and extent of the primary tumor, N indicates the involvement of nearby lymph nodes, and M signifies the presence of distant metastasis. Understanding the cancer stage is crucial for determining the most appropriate treatment approach.
Grading the Tumor
The grade of a tumor refers to how much the cancer cells differ from normal cells under a microscope. Bladder cancer is typically graded as low-grade or high-grade. Low-grade tumors grow slowly and are less likely to spread, while high-grade tumors are more aggressive and have a higher risk of metastasis. The tumor grade helps predict the cancer’s behavior and guide treatment decisions.
Prognostic Factors
Several factors influence the prognosis of metastatic bladder cancer, including the cancer’s stage and grade, the patient’s overall health, and the response to treatment. Prognostic factors help in estimating the likely course and outcome of the disease. While metastatic bladder cancer is challenging to treat, advancements in medical research continue to improve the understanding and management of this condition.
Treatment Options
Surgery
Surgical intervention is a standard treatment option for bladder cancer. For localized tumors, transurethral resection of the bladder tumor (TURBT) is often performed to remove the cancerous tissue. In cases of muscle-invasive or metastatic bladder cancer, more extensive surgery, such as radical cystectomy (removal of the bladder), may be necessary. Surgery can be combined with other treatment modalities to improve outcomes.
Chemotherapy
Chemotherapy uses powerful drugs to kill cancer cells and is a standard treatment for metastatic bladder cancer. It can be administered before surgery (neoadjuvant chemotherapy) to shrink tumors, after surgery (adjuvant chemotherapy) to eliminate remaining cancer cells, or as the primary treatment for advanced stages. Standard chemotherapy regimens include combinations of drugs such as cisplatin and gemcitabine.
Radiation Therapy
Radiation treatment utilizes high-energy bars to target and annihilate disease cells.. It can be used as a primary treatment for localized bladder cancer or in combination with other treatments for advanced stages. Radiation therapy helps control the growth of tumors, relieve symptoms, and improve the patient’s quality of life. The specific approach to radiation therapy depends on the cancer’s location and extent.
Targeted Therapy and Immunotherapy
Introduction to Targeted Therapy
Targeted therapy involves using drugs or other substances to target cancer cells while minimizing damage to normal cells. These therapies focus on molecular changes that drive cancer growth and progression. In bladder cancer, targeted therapies such as FGFR inhibitors have shown promise in treating specific disease subtypes.
Role of Immunotherapy
Immunotherapy outfits the body’s resistant framework to perceive and go after malignant growth cells. Immune checkpoint inhibitors, such as pembrolizumab and atezolizumab, have been approved for the treatment of metastatic bladder cancer. These drugs help the immune system to identify and destroy cancer cells more effectively. Immunotherapy represents a significant advancement in the treatment of bladder cancer, offering new hope for patients with advanced disease.
Clinical Trials and Emerging Treatments
Clinical trials play a crucial role in advancing the understanding and treatment of metastatic bladder cancer. These trials evaluate new drugs, combinations of therapies, and innovative treatment approaches. Participating in clinical trials provides patients access to cutting-edge treatments and contributes to developing more effective therapies for future patients.
Managing Side Effects and Complications
Common Side Effects
The treatment of metastatic bladder cancer can cause various side effects, depending on the type of therapy used. Common side effects of chemotherapy include nausea, vomiting, hair loss, fatigue, and increased susceptibility to infections. Radiation therapy can cause skin irritation, bladder irritation, and bowel problems. It is essential to discuss potential side effects with the healthcare team and develop strategies to manage them.
Long-term Complications
Long-term complications of bladder cancer treatment can impact the patient’s quality of life. These may include urinary incontinence, sexual dysfunction, and changes in bowel function. Regular follow-up care and rehabilitation programs can help address these issues and improve the patient’s overall well-being.
Supportive Care Strategies
Supportive care strategies are essential for managing the physical, emotional, and psychological challenges associated with metastatic bladder cancer. These strategies may include pain management, nutritional support, physical therapy, and counseling. Palliative care, which focuses on relieving symptoms and improving the quality of life, is also an essential aspect of supportive care for patients with advanced cancer.
Lifestyle and Dietary Considerations
Nutrition and Diet
A balanced and nutritious diet is crucial for patients with metastatic bladder cancer. Proper nutrition helps maintain strength, manage treatment side effects, and support overall health. Patients are encouraged to consume fruits, vegetables, lean proteins, and whole grains. Staying hydrated and avoiding excessive alcohol and processed foods are essential dietary considerations.
Exercise and Physical Activity
Regular physical activity can benefit patients with metastatic bladder cancer by improving energy levels, reducing fatigue, and enhancing mood. Exercise programs should be tailored to the individual’s fitness level and medical condition. Walking, swimming, and yoga can effectively promote physical and mental well-being.
Mental Health and Emotional Support
Coping with a diagnosis of metastatic bladder cancer can be emotionally challenging. Patients may experience feelings of anxiety, depression, and fear. Access to mental health services, support groups, and counseling can provide valuable emotional support. Building a strong support network of family, friends, and healthcare providers is essential for navigating the journey with metastatic bladder cancer.
Living with Metastatic Bladder Cancer
- Coping Mechanisms: Practices like mindfulness, relaxation techniques, and engaging in hobbies can help manage stress and improve emotional well-being.
- Support Systems: Building a strong network of family, friends, healthcare providers, and support groups is essential for emotional and practical support.
- Ongoing Research and Treatment: Staying informed about the latest research developments and treatment options can provide hope and improve patient outcomes.
Coping Mechanisms
Living with metastatic bladder cancer requires effective coping mechanisms to manage the physical and emotional challenges. Patients can benefit from mindfulness practices, relaxation techniques, and hobbies that bring joy and fulfillment. Maintaining a positive outlook and setting realistic goals can also enhance the quality of life.
Support Systems and Resources
Support systems and resources play a vital role in the care of patients with metastatic bladder cancer. Healthcare providers, support groups, and cancer organizations offer valuable information, resources, and emotional support. Patients and their families are encouraged to seek these resources to stay informed and connected.
Future Directions and Research
Ongoing research in metastatic bladder cancer continues to explore new treatment options and improve patient outcomes. Advances in precision medicine, targeted therapies, and immunotherapy hold promise for more effective and personalized treatments. Staying informed about the latest research developments can empower patients and their families to make informed decisions about their care.
Conclusion
Metastatic bladder cancer presents significant challenges, but understanding its causes, symptoms, diagnostic procedures, and treatment options can empower patients and their families to navigate this journey with greater confidence. Early detection, effective management of side effects, and supportive care are crucial in improving quality of life. With ongoing research and advancements in targeted therapy and immunotherapy, there is hope for better outcomes and new treatment possibilities, offering patients a chance to live more fulfilling lives despite the diagnosis.
FAQs About Metastatic Bladder Cancer
What are the early signs of metastatic bladder cancer?
Early signs include blood in the urine, frequent or painful urination, and lower back pain.
How is metastatic bladder cancer diagnosed?
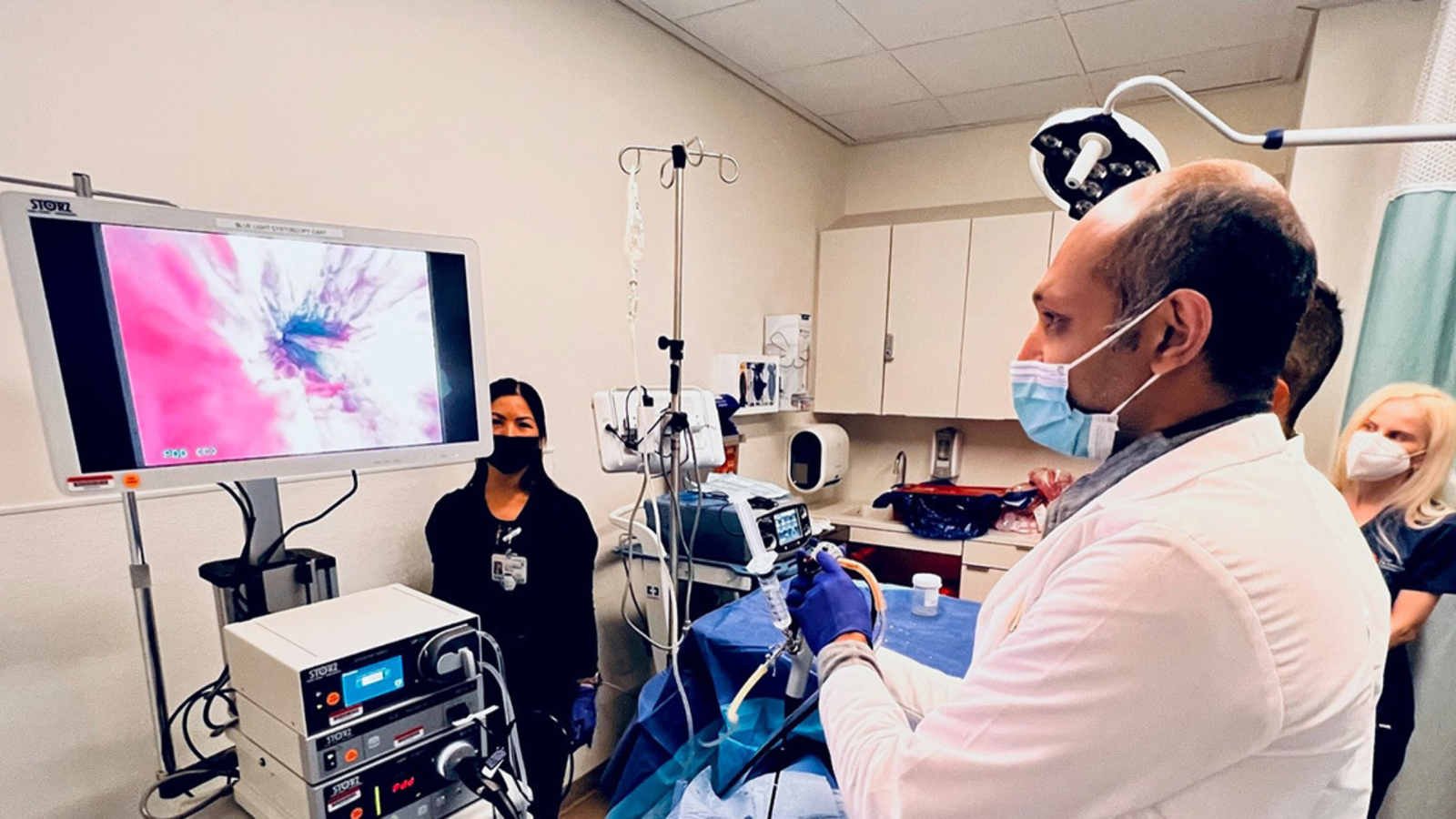
Diagnosis involves imaging techniques, cystoscopy, and biopsy.
What treatment options are available for metastatic bladder cancer?
Therapies incorporate a medical procedure, chemotherapy, radiation treatment, designated treatment, and immunotherapy.
Can lifestyle changes help manage metastatic bladder cancer?
Maintaining a healthy diet, regular exercise, and mental health support can improve overall well-being.
What is the role of immunotherapy in treating metastatic bladder cancer?
Immunotherapy helps the immune system recognize and attack cancer cells, offering a promising treatment option for advanced stages.